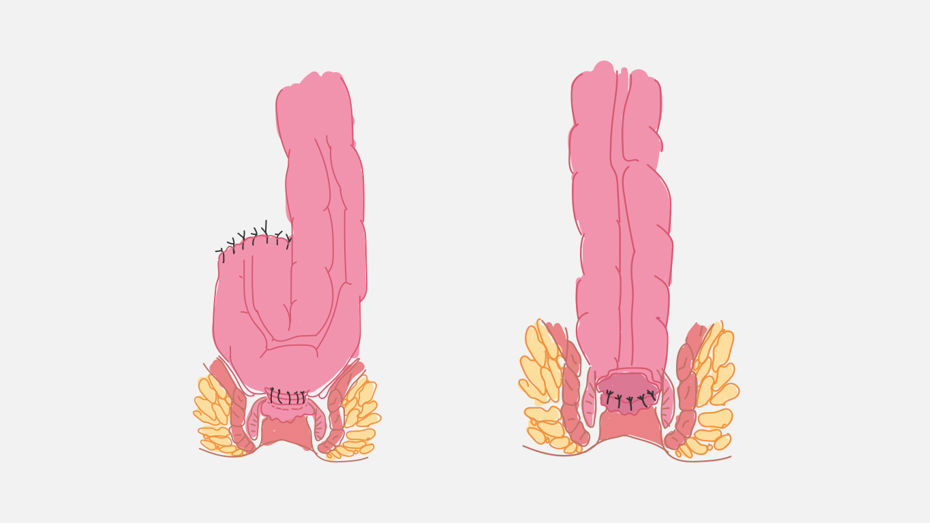
Low Anterior Resection is a surgery to remove cancer of the rectum. The part of rectum containing the tumor is removed and the remaining part of the rectum is reconnected to the colon. The surgical procedure saves the sphincter in up to 90% of the surgeries and by that avoids permanent colostomy.
This may make the patient think that their bowel function will not be affected and patients will often be informed that they will be able to have normal bowel movements post surgery.
Up to 80% of patients will however experience low anterior resection syndrome (LARS). LARS is a group of symptoms including incontinence, frequency, urgency, or feelings of incomplete emptying. Some patients may experience one of the symptoms, and some several or all of the symptoms.
LARS has a significant impact on quality of life. The pathophysiological mechanisms for LARS are likely multifactorial: internal anal sphincter (IAS) dysfunction, decrease in anal canal sensation, disappearance of the rectoanal inhibitory reflex (RAIR), disruption in local reflexes between the anus and the neorectum (neorectum is the artificial rectum constituted by a part of the colon after resection of rectum), and reduction in rectal reservoir capacity and compliance.
Treating LARS
Non-invasive methods such as biofeedback and serotonin receptor antagonists have been shown to improve symptoms, but if that does not help, TAI has been proven an effective way to improve function in patients with LARS, and also improve quality of life.
There are some different surgical reconstruction techniques to reduce LARS. However, the distal colon and rectum is normally controlled by the autonomic nervous system; parasympathetic, sympathetic and enteric acting together, and during a standard resection for rectal cancer parasympathetic and sympathetic fibers are transected. This leaves the control of the remaining bowel and neorectum to the enteric nervous system and this will affect its functionality. Sacral nerve stimulation (SNS) has been shown in some studies to decrease fecal incontinence episodes and improve quality of life for LARS patients.
Transanal irrigation for LARS
There are several studies that support the use of TAI to improve symptoms of LARS. The recommendation is to use a rectal cone instead of a rectal catheter for LARS patients to not challenge the colonic anastomosis excessively. It is also recommended to start with a low volume of irrigation fluid and then progress to a higher volume if there is inadequate response.